Research at a Glance
- Role
- Qualitative Research Lead - interview design, recruitment, synthesis, journey mapping
- Timeline
- 1 year (graduate service design project)
- Team
- 4 researchers/designers - I led the qualitative research strand
- Methods
- Semi-structured interviews, empathy mapping, journey mapping, thematic synthesis, concept testing
- Participants
- 12 parents and caregivers of children under 5
- Outcomes
- Conceptual: three service concepts validated through research; shifted team direction from content tool to human-centered service
Why This Research Mattered
Parents of young children make dozens of health decisions with incomplete information. Existing tools (symptom checkers, WebMD, parenting forums) increase anxiety more than they reduce it. We wanted to understand what actually helps parents feel confident enough to act - not just informed enough to worry more.
Context and Constraints
This was a team project in grad school. We didn't ship anything - it was conceptual. But the research was real. We had 10 weeks, a team of four, and access to parents through community groups and pediatric waiting rooms. The constraint: we couldn't observe actual medical decisions in real-time, so we relied heavily on recall interviews.
That limitation turned out to be useful. Parents remembered the emotional experience more vividly than the clinical details - and the emotional experience was where the design opportunity lived.
Research Questions
- What do parents actually do when their child has a non-emergency health concern?
- Where does trust break down in the information-seeking process?
- What would make parents feel confident enough to act instead of spiral?
Research Approach
Interviews (12 parents). I asked parents to walk me through the last time they worried about their child's health. Not hypotheticals - real moments. "Tell me about 2am. What did you do first? Then what?" The specificity surfaced behaviors that general questions miss.
Journey mapping. We mapped each parent's decision path: where they went first, what made them trust (or distrust) what they found, where they gave up or escalated. The patterns were consistent across all 12 interviews.
Thematic synthesis. I coded for trust signals, anxiety triggers, decision points, and workarounds. Three themes emerged that redirected our entire design approach.
Key Findings
Finding 1: Information increased anxiety. Every parent we talked to Googled symptoms. Every single one felt worse after. More information didn't lead to better decisions - it led to more doubt. One mom described searching "baby rash dangerous" at 3am, getting 47 different answers, and just crying.
Finding 2: Parents wanted a person, not a tool. When I asked "what would actually help?", the answer was consistent: someone who could listen, understand context, and say "here's what I'd do." Not an algorithm. A person.
Finding 3: Trust depended on perceived understanding. Parents trusted sources that acknowledged their specific situation, not generic advice. "Your 8-month-old with a 101 fever after vaccination" was trusted. "Fever in infants" was not.
How Research Changed Our Direction
We started with the assumption that parents needed better information. The research said the opposite: they needed less information and more human connection.
That shifted our entire approach. Instead of designing another symptom-checker, we designed three service concepts around human access:
- 24/7 nurse hotline - voice and text access to someone who can contextualize symptoms
- Mobile pediatric clinic - pop-up access for underserved communities who can't easily get to a doctor
- Companion app - not for diagnosis, but to help parents prepare questions before doctor visits so they feel heard
None of these were revolutionary ideas. But the research gave us permission to prioritize human connection over feature lists.
Design Concepts (Team Prototypes)
The team explored service concepts informed by research:
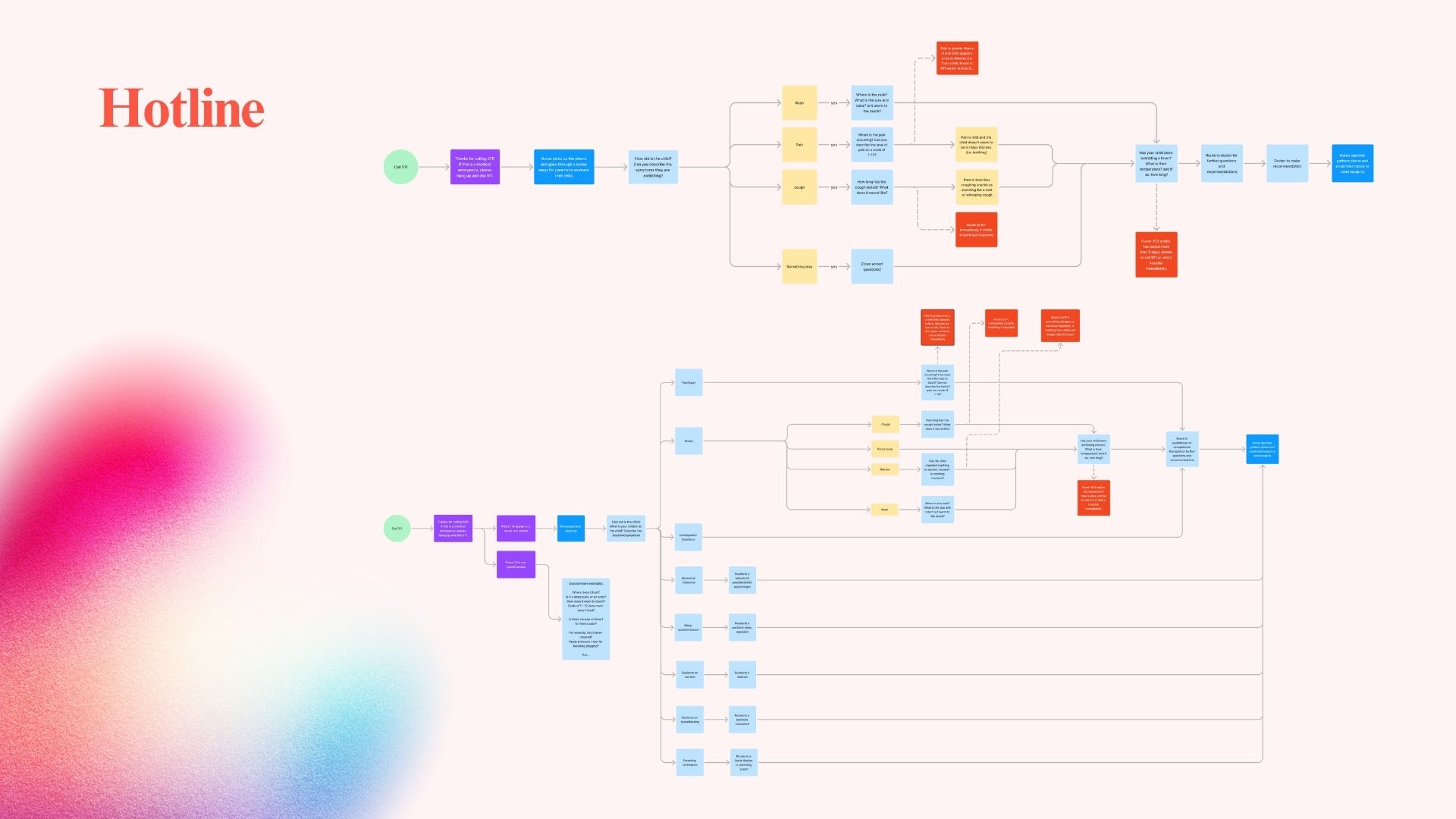
- 24/7 Parent Hotline - Phone and text access to nurses and pediatric professionals
- Mobile Pediatric Clinic - Pop-up clinics for underserved urban and rural areas
- Companion Mobile App - Appointment context, location, and medical history intake
Concepts prioritized accessibility, clarity, and trust over feature complexity.
Project Visuals
Research & process

Concept & synthesis


Prototype & outcome

Impact (Conceptual Outcomes)
(Academic concept project - percentage-based outcomes derived from qualitative synthesis)
What stayed with me
Sometimes the best design isn't a feature. It's access to a real person who can help.
Figma · Canva · UX Research Methods · Service Design
Project Video (My Contribution)
Short walkthrough explaining my UX research contribution and design rationale. Watch on Vimeo or available upon request.